Cognitive approaches
Cognitive approaches to working with voices focus on addressing people’s thoughts or beliefs about their voice-hearing experiences. In this section, we cover two different types of cognitive approach: Cognitive Behavioural Therapy (CBT) and Cognitive Analytical Therapy (CAT). We have grouped them together because they are both forms of talking therapy that are aimed at changing how people think about their voices in order to help them find better ways of coping when the voices are distressing.
Cognitive behavioural therapy (CBT)
- CBT mostly focuses on thinking and behaviour in the ‘here and now’.
- CBT for psychosis would usually be offered by a psychologist and could be one-to-one or run in a group.
- Often the aim would be to make voices feel less distressing.

Someone who is looking for support for their voices from the NHS might be offered CBT for Psychosis.
This kind of CBT usually involves meeting with a for roughly 8-16 sessions and talking to them about unusual experiences (like voices or visions) and unusual thoughts and feelings. That might include talking about what the voices say when they tend to happen, and how they make someone think and feel. Sometimes there is ‘homework’ between the sessions (e.g. keeping a diary about thoughts and voices). In general, the focus is what can be done in the here and now.
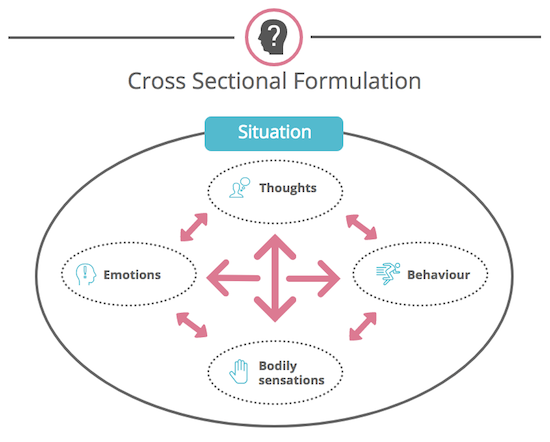
CBT often involves developing something called a : this is a kind of framework or explanation that links together thoughts, feelings, experiences and behaviour. The aim is to understand how things started to become a problem and how that might be changed. The and the person doing the therapy should develop this in collaboration; it should lead to a shared understanding that can be used to identify things to try to change. Formulations can often look like vicious circles or flowcharts.
CBT tends to focus on finding patterns in our thoughts and behaviour and how they interact with the problem at hand. For voices, this might involve thinking about what things might act as a trigger (such as the stress of poor sleep) and what kinds of patterns of thinking happen when the voices are around.
Stopping the voices completely would not usually be an aim of CBT, but it might help someone to think differently about the experience. For example, understanding more about when the voices are likely to occur might make them feel more controllable or less powerful.
This is a video designed for training therapists, but it provides an example of what a CBT session on voices can involve (Psychosis Research Unit, 2015).
In practice this does not always happen, and it can vary a lot from service to service. There may also be a waiting list to see a psychologist. In some areas group-based or computer-based CBT might also be available (which can allow more people have access).
- It can help to gain a different perspective on experiences that are unusual or hard to explain
- It can help to make voices feel more normal, or to realise how many people it happens to
- It can make someone feel listened to and in an equal partnership with the therapist
- It can help to “map out” what’s going on for someone hearing voices (on the inside and outside)
As with any talking therapy, how useful CBT will feel depends on the people involved and what kinds of expectations they have. It’s also important to note that CBT for psychosis is not just about voices: for some people this will be fine, but others might want a more tailored approach.
In February last year, 10 years since being diagnosed, I finally started psychological therapy treatment. I went to the Maudsley Hospital in London every week for sessions of CBT and the therapist helped me to find strategies to cope. I have really bad problems sleeping and CBT has helped with this and really helped with the ‘nasty voice’. CBT has helped me remain aloof from this voice and I no longer believe what it says. I now think of the voice as a petty bully and don’t let it bother me. It’s all about taking back control. The difference CBT has made is amazing – it has really transformed my life … The only thing I regret is that I didn’t have access to it sooner – it could have prevented a lot of suicide attempts and I wouldn’t have felt so awful for so long.
David Strange
I am doing CBT – the P one for psychosis. It kind of gives you false hope because it gives you all these techniques or tools that kinda work in this specific setting but when you’re living in the real world and you get challenged with this, you’re not going to be thinking ‘oh how can I challenge this or let me challenge this’. You are caught off guard and your brain is just trying to survive. You’ve got this thing trying to tear you apart. It’s very difficult to have a clear head in those situations.
Conor*
Where next?
Over the years, CBT has changed quite a lot and it can involve a range of ideas from other therapies. You might find it interesting to have a look at Cognitive Analytical Therapy, Compassion-Focused Therapy and Acceptance and Commitment therapy.
Find out more
Read
Lucy Maddox (2014). What is CBT for psychosis anyway? The Guardian.
Alison Brabban et al (2016). The importance of human relationships, ethics and recovery-orientated values in the delivery of CBT for people with psychosis. Psychosis. An academic paper that reviews research on how people experience CBT for psychosis, featuring a number of quotes from service-users. See also this post on the Mental Elf blog from 2014.
Watch
MIND (2015). What is CBT? Making sense of cognitive behavioural therapy. A general video about CBT developed by the mental health charity MIND.
David Kingdon (2013). Cognitive Therapy for Psychosis – Voices. A short talk from Professor David Kingdon on CBT for voices.
Alison Brabban (2017). Improving Access to Psychological Therapies (IAPT) for Psychosis.
Cognitive analytical therapy (CAT)
CAT is occasionally offered alongside, or instead of CBT. CAT complements the use of CBT as they both use a cognitive approach. However, CAT offers a deeper understanding of the relationship that an individual can have, not only with their thoughts, behaviours and feelings, but with the past, other people and the world around them. This can provide a more in-depth insight into why specific problems have occurred in a person’s life and how they might be linked to voice-hearing experiences.
There are CAT practitioners and psychotherapists in the but not all localities have CAT services. CAT may be available within some voluntary organisations providing therapy services (e.g. ASPIRE Community Links in Leeds), through private healthcare associations, and some university counselling services. A list of accredited CAT therapists is available here.
For more information, visit the Association for Cognitive Analytical Therapy website.